Vox clamantis in deserto
Regions in search of a country
See “The Nine Nations of North America,’’ by Joel Garreau
— Map by A Max J -
From Robert Whitcomb’s “Digital Diary,’’ in GoLocal24.com
Colin Woodard’s book Union: The Struggle to Forge the Story of United States Nationhood is at its core a narrative of how wishful thinking, racism and willful ignorance led historians to promote pictures of America that ignored the huge impact of slavery/Jim Crow and regionalism. (Note that a previous Woodard book was entitled American Nations.)
He sees the United States as having developed mostly region by region -- politically, economically and culturally -- and not in a unitary way. Consider “Greater New England’’; the Planter Class of Tidewater Virginia and Maryland down to Georgia, and the tough Scots-Irish in the Border States and interior South. The caste system that developed with slavery had a great deal to do with how the last two groups turned out.
Mr. Woodard mostly tells his tale through biographies of five people: New England’s George Bancroft (1800-1891), a very intellectually dishonest but popular historian; South Carolina writer and politician William Gilmore Simms (1806-1870), a romanticist of the slave-owning South, especially its “aristocratic’’ coastal Planter Class; Frederick Douglass (1818-1895) the great abolitionist, orator and writer; historian Frederick Jackson Turner (1861-1932), whose theories about sectionalism and the role of the frontier revolutionized the teaching of American history, and Woodrow Wilson (1856-1924), the deeply racist president, political scientist and popular historian.
After reading this book I was again reminded of how it still sometimes seems more a collection of quasi-countries than a unified country. Just look at our national elections up to last November!
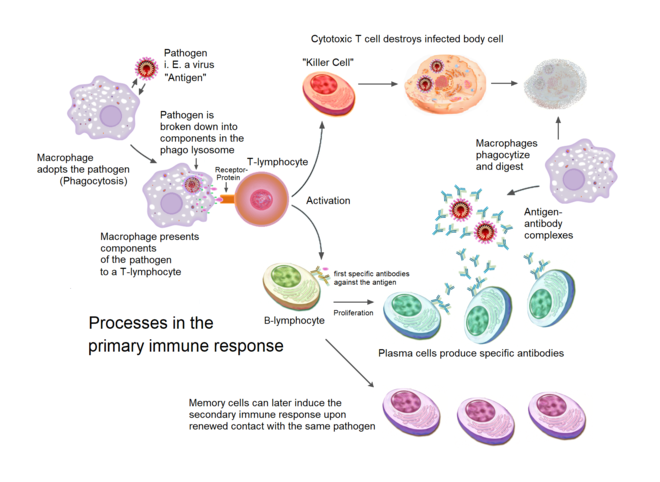
Liz Szabo: COVID-19 can disrupt the immune system in very dangerous ways
-Graphic by Sciencia58
“These are the air traffic controllers,” If these proteins are disrupted, “your immune system doesn’t work properly.”
— Aaron Ring, M.D., assistant professor of immunology at the Yale School of Medicine
There’s a reason soldiers go through basic training before heading into combat: Without careful instruction, green recruits armed with powerful weapons could be as dangerous to one another as to the enemy.
The immune system works much the same way. Immune cells, which protect the body from infections, need to be “educated” to recognize bad guys — and to hold their fire around civilians.
In some C0VID patients, this education may be cut short. Scientists say unprepared immune cells appear to be responding to the coronavirus with a devastating release of chemicals, inflicting damage that may endure long after the threat has been eliminated.
“If you have a brand-new virus and the virus is winning, the immune system may go into an ‘all hands on deck’ response,” said Dr. Nina Luning Prak, co-author of a January study on covid and the immune system. “Things that are normally kept in close check are relaxed. The body may say, ‘Who cares? Give me all you’ve got.’”
While all viruses find ways to evade the body’s defenses, a growing field of research suggests that the coronavirus unhinges the immune system more profoundly than previously realized.
Some covid survivors have developed serious autoimmune diseases, which occur when an overactive immune system attacks the patient, rather than the virus. Doctors in Italy first noticed a pattern in March 2020, when several covid patients developed Guillain-Barré syndrome, in which the immune systems attacks nerves throughout the body, causing muscle weakness or paralysis. As the pandemic has surged around the world, doctors have diagnosed patients with rare, immune-related bleeding disorders. Other patients have developed the opposite problem, suffering blood clots that can lead to stroke.
All these conditions can be triggered by “autoantibodies” — rogue antibodies that target the patient’s own proteins and cells.
In a report published in October, researchers even labeled the coronavirus “the autoimmune virus.”
“Covid is deranging the immune system,” said John Wherry, director of the Penn Medicine Immune Health Institute and another co-author of the January study. “Some patients, from their very first visit, seem to have an immune system in hyperdrive.”
Although doctors are researching ways to overcome immune disorders in covid patients, new treatments will take time to develop. Scientists are still trying to understand why some immune cells become hyperactive — and why some refuse to stand down when the battle is over.
Key immune players called “helper T cells” typically help antibodies mature. If the body is invaded by a pathogen, however, these T cells can switch jobs to hunt down viruses, acting more like “killer T cells,” which destroy infected cells. When an infection is over, helper T cells usually go back to their old jobs.
In some people with severe covid, however, helper T cells don’t stand down when the infection is over, said James Heath, a professor and president of Seattle’s Institute for Systems Biology.
About 10% to 15% of hospitalized COVID patients Heath studied had high levels of these cells even after clearing the infection. By comparison, Heath found lingering helper T cells in fewer than 5% of covid patients with less serious infections.
In affected patients, helper T cells were still looking for the enemy long after it had been eliminated. Heath is now studying whether these overzealous T cells might inflict damage that leads to chronic illness or symptoms of autoimmune disease.
“These T cells are still there months later and they’re aggressive,” Heath said. “They’re on the hunt.”
COVID appears to confuse multiple parts of the immune system.
In some patients, covid triggers autoantibodies that target the immune system itself, leaving patients without a key defense against the coronavirus.
In October, a study published in Science led by Rockefeller University’s Jean-Laurent Casanova showed that about 10% of covid patients become severely ill because they have antibodies against an immune system protein called interferon.
Disabling interferon is like knocking down a castle’s gate. Without these essential proteins, invading viruses can overwhelm the body and multiply wildly.
New research shows that the coronavirus may activate preexisting autoantibodies, as well as prompt the body to make new ones.
In the January study, half of the hospitalized covid patients had autoantibodies, compared with fewer than 15% of healthy people. While some of the autoantibodies were present before patients were infected with SARS-CoV-2, others developed over the course of the illness.
Other research has produced similar findings. In a study out in December, researchers found that hospitalized covid patients harbored a diverse array of autoantibodies.
While some patients studied had antibodies against virus-fighting interferons, others had antibodies that targeted the brain, thyroid, blood vessels, central nervous system, platelets, kidneys, heart and liver, said Dr. Aaron Ring, assistant professor of immunology at Yale School of Medicine and lead author of the December study, published online without peer review. Some patients had antibodies associated with lupus, a chronic autoimmune disorder that can cause pain and inflammation in any part of the body.
In his study, Ring and his colleagues found autoantibodies against proteins that help coordinate the immune system response. “These are the air traffic controllers,” Ring said. If these proteins are disrupted, “your immune system doesn’t work properly.”
COVID patients rife with autoantibodies tended to have the severest disease, said Ring, who said he was surprised at the level of autoantibodies in some patients. “They were comparable or even worse than lupus,” Ring said.
Although the studies are intriguing, they don’t prove that autoantibodies made people sicker, said Dr. Angela Rasmussen, a virologist affiliated with Georgetown’s Center for Global Health Science and Security. It’s possible that the autoantibodies are simply markers of serious disease.
“It’s not clear that this is linked to disease severity,” Rasmussen said.
The studies’ authors acknowledge they have many unanswered questions.
“We don’t yet know what these autoantibodies do and we don’t know if [patients] will go on to develop autoimmune disease,” said Dr. PJ Utz, a professor of immunology and rheumatology at Stanford University School of Medicine and a co-author of Luning Prak’s paper.
But recent discoveries about autoantibodies have excited the scientific community, who now wonder if rogue antibodies could explain patients’ differing responses to many other viruses. Scientists also want to know precisely how the coronavirus turns the body against itself — and how long autoantibodies remain in the blood.
‘An Unfortunate Legacy’
Scientists working round-the-clock are already beginning to unravel these mysteries.
A study published online in January, for example, found rogue antibodies in patients’ blood up to seven months after infection.
Ring said researchers would like to know if lingering autoantibodies contribute to the symptoms of “long COVID,” which afflicts one-third of covid survivors up to nine months after infection, according to a new study in JAMA Network Open.
“Long haulers” suffer from a wide range of symptoms, including debilitating fatigue, shortness of breath, cough, chest pain and joint pain, according to the Centers for Disease Control and Prevention. Other patients experience depression, muscle pain, headaches, intermittent fevers, heart palpitations and problems with concentration and memory, known as brain fog.
Less commonly, some patients develop an inflammation of the heart muscle, abnormalities in their lung function, kidney issues, rashes, hair loss, smell and taste problems, sleep issues and anxiety.
The National Institutes of Health has announced a four-year initiative to better understand long covid, using $1.15 billion allocated by Congress.
Ring said he’d like to study patients over time to see if specific symptoms might be explained by lingering autoantibodies.
“We need to look at the same patients a half-year later and see which antibodies they do or don’t have,” he said. If autoantibodies are to blame for long covid, they could “represent an unfortunate legacy after the virus is gone.”
Widening the Investigation
Scientists say the coronavirus could undermine the immune system in several ways.
For example, it’s possible that immune cells become confused because some viral proteins resemble proteins found on human cells, Luning Prak said. It’s also possible that the coronavirus lurks in the body at very low levels even after patients recover from their initial infection.
“We’re still at the very beginning stages of this,” said Luning Prak, director of Penn Medicine’s Human Immunology Core Facility.
Dr. Shiv Pillai, a Harvard Medical School professor, notes that autoantibodies aren’t uncommon. Many healthy people walk around with dormant autoantibodies that never cause harm.
For reasons scientists don’t completely understand, viral infections appear able to tip the scales, triggering autoantibodies to attack, said Dr. Judith James, vice president of clinical affairs at the Oklahoma Medical Research Foundation and a co-author of Luning Prak’s study.
For example, the Epstein-Barr virus, best known for causing mononucleosis, has been linked to lupus and other autoimmune diseases. The bacteria that cause strep throat can lead to rheumatic fever, an inflammatory disease that can cause permanent heart damage. Doctors also know that influenza can trigger an autoimmune blood-clotting disorder, called thrombocytopenia.
Researchers are now investigating whether autoantibodies are involved in other illnesses — a possibility scientists rarely considered in the past.
Doctors have long wondered, for example, why a small number of people — mostly older adults — develop serious, even life-threatening reactions to the yellow fever vaccine. Three or four out of every 1 million people who receive this vaccine — made with a live, weakened virus — develop yellow fever because their immune systems don’t respond as expected, and the weakened virus multiplies and causes disease.
In a new paper in the Journal of Experimental Medicine, Rockefeller University’s Casanova has found that autoantibodies to interferon are once again to blame.
Casanova led a team that found three of the eight patients studied who experienced a dangerous vaccine reaction had autoantibodies that disabled interferon. Two other patients in the study had genes that disabled interferon.
“If you have these autoantibodies and you are vaccinated against yellow fever, you may end up in the ICU,” Casanova said.
Casanova’s lab is now investigating whether autoantibodies cause critical illness from influenza or herpes simplex virus, which can cause a rare brain inflammation called encephalitis.
Calming the Autoimmune Storm
Researchers are looking for ways to treat patients who have interferon deficiencies — a group at risk for severe covid complications.
In a small study published in February in the Lancet Respiratory Medicine, doctors tested an injectable type of interferon — called peginterferon-lambda — in patients with early covid infections.
People randomly assigned to receive an interferon injection were four times more likely to have cleared their infections within seven days than the placebo group. The treatment, which used a type of interferon not targeted by the autoantibodies Casanova discovered, had the most dramatic benefits in patients with the highest viral loads.
Lowering the amount of virus in a patient may help them avoid becoming seriously ill, said Dr. Jordan Feld, lead author of the 60-person study and research director at the Toronto Centre for Liver Disease in Canada. In his study, four of the placebo patients went to the emergency room because of breathing issues, compared with only one who received interferon.
“If we can bring the viral levels down quickly, they might be less infectious,” Feld said.
Feld, a liver specialist, notes that doctors have long studied this type of interferon to treat other viral infections, such as hepatitis. This type of interferon causes fewer side effects than other varieties. In the trial, those treated with interferon had similar side effects to those who received a placebo.
Doctors could potentially treat patients with a single injection with a small needle — like those used to administer insulin — in outpatient clinics, Feld said. That would make treatment much easier to administer than other therapies for covid, which require patients to receive lengthy infusions in specialized settings.
Many questions remain. Dr. Nathan Peiffer-Smadja, a researcher at the Imperial College London, said it’s unclear whether this type of interferon does improve symptoms.
Similar studies have failed to show any benefit to treating patients with interferon, and Feld acknowledged that his results need to be confirmed in a larger study. Ideally, Feld said, he would like to test interferon in older patients to see whether it can reduce hospitalizations.
“We’d like to look at long haulers, to see if clearing the virus quickly could lead to less immune dysregulation,” Feld said. “People have said to me, ‘Do we really need new treatments now that vaccines are rolling out?’ Unfortunately, we do.”
Liz Szabo is a Kaiser Health News reporter.
Liz Szabo: lszabo@kff.o
Early spring
Black boughs against a pale, clear sky,
Slight mists of cloud-wreaths floating by;
Soft sunlight, gray-blue smoky air,
Wet thawing snows on hillsides bare.
–Emma Lazarus (1849–87)
Llewellyn King: Ireland -- an island of glorious contradictions that charms the world, especially on March 17
The Humbert Monument on Humbert Street in Ballina, County Mayo, Ireland. It honors Jean Joseph Amable Humbert, who was sent by Napoleon to assist the Irish with the uprising against the English in 1798.
WEST WARWICK, R.I.
Where I live things are beginning to turn green with a hint of spring. But it isn’t just the flora here that has an intimation of green. The whole country, indeed, the whole world, is greening for St. Patrick’s Day.
The most extraordinary thing happens on that day: People around the world shed their ethnic identities to take on an Irish one. On March 17, the world decides that it is Irish and that it must, as the Irish do, take a drink.
No other country commandeers the world as does that small island nation set in the North Atlantic. On the day when an otherwise obscure saint is celebrated, the world wears some item of green and quaffs something fermented or distilled.
For me, Ireland has always been a place of glorious contradictions and great writers – Joyce, Yeats, Shaw, Wilde, Swift, O’Brien, Beckett and Lewis, come to mind in no order, and there are hundreds more.
It isn’t just that its writers are among the greatest, but also that the Irish speak poetically, eschewing the simple answer, embroidering the boring cloth of fact, and sometimes confusing those who don’t have the gift of deciphering eloquence.
An Irish friend, John McCaughey, and I were walking with our wives in Kinsale, on the southwest coast of Ireland, when we came upon a tempting pub and were tempted. It wasn’t open, but an old man – and the old men of Ireland are a breed apart -- was patiently waiting.
“When will he be open?” John asked.
“He’d hardly be open now,” said the old man.
“Well, when will he be open?”
“Oh, he’ll be open in good time.”
I asked John what he meant by “in good time.”
It means, said John, that he didn’t have a clue, but he wouldn’t like to say something so bald and down-letting.
In Ireland, the facts are often delivered in fine gift-wrapping.
In a restaurant, my wife asked whether the fish was fresh. The waiter replied, “If it were any fresher, it would be swimming, and you wouldn’t want that now, would you?”
I spent two decades visiting Ireland as the American organizer of the Humbert Summer School in Ballina, County Mayo. Summer schools in Ireland are study groups that meet once a year and can focus on literature, like the Yeats school, or politics like the Parnell school. They are akin to Bill Clinton’s Renaissance weekends.
The Humbert Summer School, created by John Cooney, the eminent historian and journalist, and sadly no longer operating, was named for Gen. Jean Joseph Amable Humbert, who was sent by Napoleon to assist the Irish with the uprising against the English in 1798, remembered in The Year of the French, by Thomas Flanagan. The uprising failed, but Humbert became an Irish hero. (He fought gallantly in the Battle of New Orleans and ended his days in the city as French teacher.)
Our summer school examined the position of Ireland in the world, especially its role in Europe. Every year I would try and bring a few Americans to the northwest of Ireland to enjoy the discussions, the great lamb, salmon and potatoes, and, of course, the free flow of Guinness, Murphy’s (another stout), Smithwick’s (the dominant beer), and Bushmills and Jameson whiskeys, refreshments we found conducive to good talk.
That part of Ireland historically had been hard used by the English, from the time of William of Orange in the 17th Century to the Black and Tans in 1920, who were ill-trained and equipped English policemen, many teenagers, raised in England and inserted into the Royal Irish Constabulary, to oppose the Irish fight to overthrow English rule. They wore surplus green tunics and khaki trousers. Their conduct was brutal and thuggish.
I had told this dreadful history of English oppression in some detail to one of my American guests, Ray Connolly, who was from Boston. Driving back to Dublin, after the summer school session, we stopped at a pub. When the publican heard my English accent, he asked me about the weather “over there.” I knew that he meant England. I told him that I used to live in England, but I had lived in the United States for many years and had become an American citizen. Rather than curling his lip at me, he threw his arms around my neck and said, “God bless you. You haven’t lost your accent.”
My friend looked surprised. I explained to Ray that the Irish love to denounce the English, but they are especially proud when their children have homes and careers in London.
In Ireland, your enemy can also be your friend. That is why I shall wear the green on the great day and sip something stronger than usual and celebrate a Frenchman who fought with the Irish against my ancestors. Slainte!
Llewellyn King is executive producer and host of White House Chronicle, on PBS. His email is llewellynking1@gmail.com, and he’s based in Rhode Island and Washington, D.C.
Boston negativity 'sucks'
Rick Pitino in a press conference for the 2013 Final Four when he was head coach at the University of Louisville
“The only thing we can do is work hard, and all the negativity that’s in this town {Boston) sucks.’’
— Rick Pitino (born 1952), basketball coach at colleges (including Providence College) and the NBA (including the New York Knicks and the Boston Celtics.
The Celtics hired him as head coach in 1997. He resigned in 2001, after a 102-146 record.
Contemplating climate change on Peaks Island
“Taking a Break” (video still), by Krystal Brown, in her show “15,000 Days’,’ at Kingston Gallery, Boston, through March 28.
The gallery says Ms. Brown “contemplates climate change through the context of suspended time and death as a question rather than a finality. In this three-channel video installation, filmed November 2020 at Peaks Island, Maine, Brown utilizes conceptual motifs such as grave digging and specific costuming to speak to working-class labor, mostly the unseen work. Sound is an equally important component to the visuals of shoveled earth and a churning sea. The original poem, written by Brown, also titled “15,000 Days,’’ is performed by local Boston artist Kimberly Barnes. Experimental sound artist Adam Giangregorio provides minimalist drone music, recorded on-site at Battery Steele at Peaks Island. Through the lens of hauntology, Brown both pushes back against and concedes to an undetermined future.’’
Postcard from around 1900 showing the long-gone Gem Theater and the Peaks Island House hotel. Peaks Island is part of Portland. Its population rises from around 900 in the winter to several thousand in the summer because of people “from away” with summer houses there.
Intended for loss
Elizabeth Bishop in 1964
“The art of losing isn’t hard to master;
so many things seem filled with the intent
to be lost that their loss is no disaster.’’
— From “One Art,’’ by Elizabeth Bishop (1911-1979), considered one of the greatest American poets. She was born in Worcester and died in Boston and lived in many places in-between.
After seeing all that in Boston....
Mark Wahlberg
“It’s weird: I’ve been to prison, I’ve seen the worst sort of violence and negative shit on the streets, but when it comes to putting my heart on the line and letting somebody get to know me in a relationship, it’s very difficult.’’
— Mark Wahlberg (born 1971), movie and TV actor, producer and former rapper, was brought up on the then mean streets of Boston’s Dorchester section, where he got into drugs and crime.
Classic Boston area three-decker
In the Uphams Corner section of Dorchester showing a typical streetscape in the neighborhood (2010)
More efficient and more expensive?
“The Big Fish Eat the Small Ones,’’ by Peter Brueghel the Elder (1556).
From Robert Whitcomb’s “Digital Diary,’’ in GoLocal24.com
“The sooner patients can be removed from the depressing influence of general hospital life the more rapid their convalescence.’’
-- Charles H. Mayo, M.D. (1865-1939), American physician and a co-founder of the Mayo Clinic, in Rochester, Minn.
The plan for Lifespan and Care New England (CNE) to merge, if regulators approve it, would probably make Rhode Island health care more efficient. It would do this through integrating their hospitals and other units. That would do such things as speeding the sharing of patient information among health-care professionals and streamlining billing. Further, it would probably strengthen medical research and education in the state, much of it through the new enterprise’s very close links with the Alpert Medical School at Brown University, which, indeed, has pledged to provide at least $125 million over five years to help develop an “academic health system’’ as part of the merger.
The deal, by reducing some red tape (with the state having just one big system instead of two), might make health care in our region more user-friendly for patients, dissuading more of them from going to Boston’s world-renowned medical institutions, thus keeping more of their money here.
The best example of where the merger could improve health care would be in better connecting Lifespan’s Hasbro Children’s Hospital with Care New England’s Bradley Hospital, a psychiatric institution for children, and Women & Infants Hospital.
But would the huge (especially for such a tiny state) new institution have such power that it would impose much higher prices? Studies have shown that hospital mergers almost inevitably mean higher prices. So insurance companies, as well as poorly insured patients, may eye a Lifespan-CNE merger with trepidation.
And expect job losses, at least for a while, given the need to eliminate the administrative redundancies created by mergers. Meanwhile, senior- executive salaries in the new entity would probably be even more stratospheric than they are now at the separate “nonprofit” companies, and I imagine the golden parachutes for departing excess senior execs would blot out the sun.
Meanwhile, Boston will remain a magnet for health care, and so it’s conceivable that the behemoth and very prestigious Mass General Brigham hospital group would end up absorbing the Lifespan-CNE giant in the end anyway.
'Wonderscapes' in Framingham
“Hide and Seek” (full-room installation), by Adria Arch, in the Danforth Art Museum's (Framingham, Mass.) group exhibit, “Wonderscapes,’’ March 20-June 12
— Photo by Will Howcroft
The museum’s director, Jessica Roscio, says of the show:
“Using circles, organic forms, and undefined borders, five multi-media artists working across media create their own wonderscapes. They use the tactile nature of their materials to convey hazy, stream-of-consciousness, otherworldly dreamscapes based in reality but largely products of the mind. In focusing on elemental forms, each of these artists crafts their own narratives about time and space and the ways in which we visualize, cope, and move through our own ‘wonderscapes.’’’
When they want their nanny.
An old wet nurse symbolizing France as nanny-state and public-health provider (color photomechanical reproduction of a lithograph editorial cartoon by N. Dorville, 1901)
“When faced with economic uncertainty, people don’t want freedom. When they can’t see their economic future, they want the nanny state.’’
— John McLaughlin (1927-2016) a Providence native and one-time Jesuit priest who became a well-known conservative writer and public-affairs talk show host, best known for running The McLaughlin Group. His forceful and abrupt style was much parodied.
John McLaughlin with President Richard Nixon on May 3, 1974. Mr. McLaughlin wrote speeches for Nixon, who resigned in the Watergate scandal on Aug. 8, 1974.
Arthur Allen/Liz Szabo: Don't be picky about a COVID-19 vaccine
Boston’s Beth Israel Deaconess Medical Center, where the Johnson & Johnson COVID-19 vaccine was developed. Other vaccines are being offered by Pfizer and Cambridge-based Moderna, which is making most of its vaccines in Massachusetts. Pfizer also has major operations, like Moderna, in Cambridge’s Kendall Square area.
Meanwhile, the Novavax vaccine should be available within the next couple of months.
When getting vaccinated against COVID-19, there’s no sense being picky. You should take the first authorized vaccine that’s offered, experts say.
The newest COVID vaccine on the horizon, from Johnson & Johnson, is probably a little less effective at preventing sickness than the two shots already being administered around the U.S., from Pfizer-BioNTech and Moderna. On Saturday, the Food and Drug Administration authorized the Johnson & Johnson vaccine after reporting it showed about 66% effectiveness at preventing covid illness in a 45,000-person trial. No one who received the vaccine was hospitalized with or died of the disease, according to the data released by the company and FDA. As many as 4 million doses could be shipped out of J&J’s warehouses beginning this week.
The J&J vaccine is similar to the shots from Moderna and Pfizer-BioNTech but uses a different strategy for transporting genetic code into human cells to stimulate immunity to the disease. The Moderna and Pfizer-BioNTech vaccines were found in trials last fall to be 94% effective in preventing illness caused by covid. They also prevented nearly all severe cases.
But the difference in those efficacy numbers may be deceptive. The vaccines were tested in different locations and at different phases of the pandemic. And J&J gave subjects in its trial only one dose of the vaccine, while Moderna and Pfizer have two-dose schedules, separated by 28 and 21 days, respectively. The bottom line, however, is that all three do a good job at preventing serious COVID.
“It’s a bit like, do you want a Lamborghini or a Chevy to get to work?” said Dr. Gregory Poland, director of the Mayo Clinic’s Vaccine Research Group, who was a paid consultant in the J&J study. “Ultimately, I just need to get to work. If a Chevy is available, sign me up.”
So while expert panels may debate in the future about which vaccine is best for whom, “from a personal and public health perspective, the best advice for now is to get whatever you can as soon as you can get it, because the sooner we all get vaccinated the better off we all are,” said Dr. Norman Hearst, a family doctor and epidemiologist at the University of California-San Francisco.
Here are five reasons you should take the J&J shot if it’s the one that’s offered to you first:
1. All three vaccines protect against hospitalization and death.
Of the 10 people who got severe disease in the Pfizer trial, nine had received a placebo, or fake vaccine; none of the 30 severe cases in the Moderna trial occurred in people who got the true vaccine. A month after receiving the Johnson & Johnson shot there were no deaths or hospitalizations in those who had been vaccinated. “The real goal is to keep people out of the hospital and the ICU and the morgue,” said Dr. Paul Offit, director of the Vaccine Education Center at Children’s Hospital of Philadelphia. “This vaccine will do that well.”
2. The efficacy levels could be a case of apples and oranges.
The data that Moderna and Pfizer-BioNTech presented to the FDA for their vaccines came from large clinical trials that took place over the summer and early fall in the United States. At the time, none of the new variants of covid — some of which may be better at evading the immune responses produced by vaccines — were circulating here. In contrast, the J&J trial began in September and was put into the arms of people in South America, South Africa and the United States.
Newly widespread variants in Brazil and South Africa appear somewhat better at evading the vaccine’s defenses, and it’s possible a new variant in California — where many J&J volunteers were enrolled — may also have that trait. The J&J vaccine was 72% effective against moderate to severe covid in the U.S. part of the trial, compared with 57% in South Africa, where a more contagious mutant virus is the dominant strain. Another vaccine, made by the Maryland company Novavax, had 90% efficacy in a large British trial, but only about 50% in South Africa. The Moderna and Pfizer-BioNTech vaccines might not have gotten the same sparkling results had they been tested more recently — or in South Africa.
“This vaccine was tested in the pandemic here and now,” said Dr. Dan Barouch, a Harvard Medical School professor whose lab at the Center for Virology and Vaccine Research at Beth Israel Deaconess Medical Center, in Boston, developed the J&J vaccine. “The pandemic is a much more complex pandemic than it was several months ago.”
Some of that difference in performance also could be attributable to different patient populations or disease conditions, and not just the mutant virus. A large percentage of South Africans carry the human immunodeficiency virus, or HIV. Chinese vaccines have performed wildly differently in countries where they were tested in recent months.
“We don’t know which vaccines are the Lamborghinis,” Poland said, “because these aren’t true head-to-head comparisons.”
3. Speed is of the essence.
To stop the spread of COVID, the mutation of the virus that causes it and the continued pummeling of the economy, we all need to be vaccinated as quickly as possible. The inadequate supply of vaccines has been felt acutely.
Dr. Virginia Banks’ s 103-year-old mother is one of the few living Americans who were around for the country’s last great pandemic — the 1918 influenza — yet she’s been unable to get a covid vaccination, said Banks, a physician with Northeast Ohio Infectious Disease Associates in Youngstown.
Patients can’t be picky about which vaccine they accept, Banks said. People “need to get vaccinated with the vaccines out today so we can get closer to herd immunity” to slow the spread of the virus.
Banks has worked hard to promote covid vaccines to skeptical minority communities, frequently appearing on local TV news and making at least two presentations by Zoom each week. Blacks to date have been vaccinated against covid at much lower rates than whites.
“There’s a downside to waiting,” said Dr. William Schaffner, a professor of preventive medicine and health policy at Vanderbilt University Medical Center. Delaying vaccination carries serious risks, given that, as of Saturday, some 2,000 Americans were still dying each day of covid.
4. The J&J vaccine appears to have some real advantages.
First, it seems to cause fewer serious side effects like the fever and malaise suffered by some Pfizer-BioNTech and Moderna vaccine recipients. High fever and dehydration are particular concerns in fragile elderly people who “have one foot on the banana peel,” said Dr. Kathryn Edwards, scientific director of the Vanderbilt Vaccine Research Program. The J&J vaccine “may be a better vaccine for the infirm.”
Many people may also prefer the J&J shot because “it’s one and done,” Schaffner said. Easier for administrators too: just one appointment to schedule.
5. The J&J vaccine is much easier to ship, store and administer.
While the Johnson & Johnson vaccine can be stored in regular refrigerators, the Pfizer-BioNTech vaccine must be kept long-term in “ultra-cold” freezers at temperatures between minus 112 degrees and minus 76 degrees Fahrenheit, according to the Centers for Disease Control and Prevention.
Both the Moderna and Pfizer-BioNTech vaccines must be used or discarded within six hours after the vial is opened. Vials of the J&J vaccine can be stored in a refrigerator and restored for later use if doses remain. “Right now we have mass immunization clinics that are open but have no vaccine,” said Offit. “Here you have a single-dose regime with easy storage and handling.”
A person’s address — not their personal preference — may determine which vaccine they receive, said E. John Wherry, director of the Institute for Immunology at the University of Pennsylvania’s Perelman School of Medicine. He pointed out that the Johnson & Johnson vaccine is a simpler choice for rural areas.
“A vaccine doesn’t have to be 95% effective to be an incredible leap forward,” said Wherry. “When we get to the point where we have choices about which vaccine to give, it will be a luxury to have to struggle with that question.”
Liz Szabo and Arthur Allen are Kaiser Health News reporters.
Arthur Allen: ArthurA@kff.org, @ArthurAllen202
Liz Szabo: lszabo@kff.org, @LizSzabo
Grey on grey
—By Knulclunk
‘‘half-past nine and warm enough
to nudge a crocus out of its benumbing
winter sleep, grey swales of greysplotched
grey on grey, erratic windswept drizzle,
the swish swash of milk- and oil trucks slashed
across my trenchsliht vision when….’’
— From “A Break in the Weather,’’ by Paul Mariani (born 1940), poet and long-time literature professor at Boston College. He lives in western Massachusetts.
'Solace' in clippervillle
Promotional image from the show called “Solace’,’ featuring works by the East Boston artist-run cooperative Atlantic Works through April 24 at the neighboring Clippership Wharf’s ClipArt Gallery, East Boston. That’s the community where many of the most famous clipper ships were built in the mid-19th Century.
Painting by James E. Buttersworth done in 1859-60 of the clipper ship Flying Cloud, built in 1850-51 at famed naval architect Donald McKay’s shipyard in East Boston.
Chris Powell: Abolish government pensions
New Haven Police Chief Otoniel Reyes is “retiring” at age 49 with a $117,000-a-year pension to move to nearby Quinnipiac University, where he’ll run the campus police at a salary that will probably be around $170,000.
MANCHESTER, Conn.
Connecticut should prohibit pensions for state and municipal government employees, not because they are bad people or especially undeserving but for several solid policy reasons.
First, most of the taxpayers who pay for those pensions don't enjoy anything like them.
Second, state and municipal government can't be trusted to fund the pensions adequately.
And third, the pension system for state and municipal employees separates a huge and politically influential group from Social Security, the federal pension system on which nearly everyone else relies, and thus weakens political and financial support for it.
Connecticut state government has an estimated $60 billion in unfunded liabilities in its state-employee and municipal-teacher pension funds. But after attending the recent meeting of the state General Assembly's finance committee, Yankee Institute investigative reporter Marc Fitch wrote that another $900 million in unfunded liabilities are sitting in New Haven's pension funds.
According to Fitch, New Haven Mayor Justin Elicker testified about the city's pension-fund disaster, noting that city government faces a projected $66 million deficit in its next budget and that pension obligations are a major cause of it.
Of course the mayor attended the hearing to beg more money from state government for the city. Unfortunately no legislator seems to have asked Elicker about the $117,000 annual pension that the city is about to start paying its police chief, Otoniel Reyes, so that he can "retire" at age 49 to take a job with Quinnipiac University, in nearby Hamden, Conn., probably at a salary around $170,000, and begin earning credit toward a second luxurious pension. Indeed, no news organization in New Haven seems to have even reported the chief's premature pension yet.
Maybe legislators didn't ask about the "retiring" chief's pension because state government has been just as incompetent and corrupt with pensions as New Haven city government. These enormous and incapacitating unfunded liabilities are proof of political corruption and incompetence at both the state and city levels -- the promising of unaffordable benefits to a politically influential special interest.
Connecticut's tax system may be unfair, but it's not why New Haven is insolvent. Like state government, the city is insolvent because it has given too much away.
Government in Connecticut is good at clearing snow from the streets and highways because failure there is immediately visible. But beyond snowplowing government, in Connecticut is not much more than a pension and benefit society whose operation powerfully distracts from serving the public.
This distraction should be eliminated, phased out as soon as government recognizes that it has higher purposes than the contentment of its own employees.
xxx
Proposing his new state budget this month, Governor Lamont announced plans to close three of Connecticut's 14 prisons in response to the decline of nearly 50 percent in the state's prison population over the last decade.
A few days later New Haven's Board of Alders asked Assistant Police Chief Karl Jacobson to explain the recent explosion of violent crime in the city.
According to the New Haven Register, the assistant chief said there were 73 gang-related shootings in the city in 2020 against only 41 in 2019 and 32 in 2018. Murders in the city so far this year total seven, against none in the same period last year. So far this year there have been 12 shootings in the city, up from five at this time last year, and 36 shooting incidents this year compared to 20 at this time last year.
As usual, the assistant chief said, a big part of the violence in the city involves men recently released from prison who resume feuds and otherwise are prone to get into trouble. The police plan to hold preventive meetings with such men, and the city has just opened a "re-entry center" for new parolees.
The explosion of crime in New Haven, Hartford, Bridgeport and other cities does not sound like cause to close prisons. It sounds like cause to investigate prison releases and the failure of criminal rehabilitation.
Maybe the General Assembly would undertake such investigation if the former and likely future offenders were delivered to suburbs instead of cities. Then saving money by closing prisons might not be considered such a boast.
xxx
Chris Powell is a columnist for the Journal Inquirer, in Manchester.
Good show for a stony region
“Water and Rocks” (print on aluminum), by Robin MacDonald-Foley, in her show “Seeing Stone,’’ at Galatea Fine Art, Boston, March 5-28.
She tells the gallery:
"Seeing Stone is a journey of exploration represented as a body of work inspired by forms and shapes found in nature. Uniting stone and stone’s relationships within the natural environment is my focus. Pairing sculpture and photography, these stone carvings and images play upon spatial relationships, intending to draw the viewer in. This work is a personal narrative, depicting the power, calm and permanence of stone.
“In my recent work, visualizing places becomes part of my sculpture. A carving of a vessel takes me on an inward journey navigating oceans and eroded facades etched in lichen stories noting the passage of time. Studying stone as an object, thoughts are captured as photographic impressions of rocks against a blue sky. Bound together by fate, they stand on their own, each central to my theme.
“My work is carved by hand in a steady rhythm of tool to stone, a challenging technique that enables me to bond with a piece over long periods of time. When its form emerges, history begins anew. Working with multiple pieces, I imagine how they connect in color and texture, allowing the placement of objects to redefine permanent qualities. Sometimes a polished finish brings the coloration of an alabaster carving to life, or a self-portrait becomes part of my setting. Sitting by the ocean, or sheltering in cave-like stone structures, my feet intuitively absorb Earth's undulating destinations. I sit quietly sharing time and space with the stone."
She lives in the town of Stoughton, south of Boston.
‘
Downtown Stoughton.
Downtown Stoughton in 1912. Even many small towns had streetcars then.
Why not leave them all on the beach?
“One cannot collect all the beautiful shells on the beach,’’ in Gift From the Sea (1955)
— Anne Morrow Lindbergh (1906-2001), best-selling essayist/author, some of whose writings presaged the Green Movement, and aviator. She was wife of aviator, inventor, military officer, Nazi sympathizer (like her for a time) and womanizing (and with simultaneous-multiple families) Charles Lindbergh. She spent her final years living near her daughter Reeve, an author herself, in the northern Vermont village of Passumpsic, part of the town of Barnet. Before then she and her husband lived off and on in Darien, Conn. (“Aryans from Darien’’), in a rich section on Long Island Sound.
The Barnet, Vt., post office
1914 postcard. But the Lindberghs were not contented.
Carey Goldberg: Boston physician named to run CDC uses data to save lives
Dr. Rochelle Walensky
BOSTON
In early December, Dr. Katy Stephenson was watching TV with her family and scrolling through Twitter when she saw a tweet that made her shout.
“I said ‘Oh, my God!'” she recalled. “Super loud. My kids jumped up. My husband looked over. He said, ‘What’s wrong, what’s wrong, is everything OK?’ I was like, ‘No, no, it’s the opposite. It’s amazing. This is amazing!'”
Dr. Rochelle Walensky had just been tapped to lead the Centers for Disease Control and Prevention.
Stephenson is an infectious-diseases specialist and vaccine scientist at Beth Israel Deaconess Medical Center, in Boston. So the news had special meaning for her and the many jubilant colleagues tweeting their joy. They’d been helping one another through the brutal pandemic year, she said, while feeling they had little to no help from the federal government.
“It was so baffling,” she said. “It wasn’t even just that we didn’t know what the government was doing. It was that sometimes it felt like sabotage. Like the federal government was actively trying to mess things up.”
But through it all, as the long months became a year, Walensky had been out front, Stephenson said, sticking to the science and telling the truth.
When Walensky stepped up to lead the CDC, she promised to keep telling the truth — even when it’s bad news. She told a JAMA Network podcast last month that she’ll welcome straight talk from the scientists at the CDC as well.
“They have been diminished,” she said. “I think they’ve been muzzled — that science hasn’t been heard. This top-tier agency, world-renowned, hasn’t really been appreciated over the last four years and really markedly over the last year, so I have to fix that.
Walensky, 51, has long been a doctor on a mission — first, to fight AIDS around the world, and now, to shore up the CDC and get the United States through the pandemic. Beyond unmuzzling her agency’s staff, she vows to tackle many other challenges, pushing particularly hard on vaccine distribution and rebuilding the public health system.
Walensky’s family has a tradition of service, including a grandfather who served in World War II and rose to be a brigadier general. And she likens the call she got from the Biden administration to a hospital alarm that goes off when a patient is in cardiac arrest.
“I got called during a code,” she told JAMA. “And when you get called during a code, your job is to be there to help.”
At Massachusetts General Hospital, where Walensky was the chief of infectious diseases, some of her many admirers now have T-shirts that read “Answer the Code” with her initials, RPW, beneath.
The shirts are part of an outpouring of affection in Boston biomedical circles and far beyond that greeted Walensky’s appointment — including a flood of floral bouquets that her husband and three sons helped accept after word of her new job got out.
“At one point, one of my sons said, ‘You know, Dad, we should just open a florist shop at this point,” said Dr. Loren Walensky, the CDC director’s husband.
He studies and treats children’s blood cancers at Boston Children’s Hospital and the Dana-Farber Cancer Institute. And now he could be called the “first gentleman” of the CDC.
He calls Rochelle his “Wonder Woman” and still remembers when he first saw her 30 years ago, in the cafeteria of the Johns Hopkins University School of Medicine, where they were both students.
“She stood out,” he said. “And one of the reasons why she stood out is because she stands tall. Rochelle is 6 feet tall.”
She also had extraordinary energy and discipline, even then, he remembered: “Most of us would roll out of bed and stumble into the lecture hall as our first activity of the day and, for Rochelle, she was already up and running and bright-eyed and bushy-tailed for hours before any of us ever saw the light of day.”
After medical school, Rochelle Walensky trained in a hospital medical unit so tough it was compared to the Marines. It was the mid-’90s, and the AIDS epidemic was raging. She saw many people die. And then, a few years later, she saw the advent of HIV treatments that could save patients — if those patients could get access to testing and care.
Loren Walensky recalls coming home one day to find her sitting at the kitchen table working on extremely complex math. She was starting to broaden her focus from patient care to bigger-picture questions about the increased equity in health care that more funding and optimal treatment choices could bring.
“And it was like a switch went off,” he said, “and she just had this natural gift for this style of testing — whether if you did X, would Y happen, and if you did X with a little more money, then how would that affect Y? And all of these if-thens.”
She started doing more research, including studies of ways to get more patients tested and treated for AIDS, even in the poorest countries. One of her most prominent papers calculated that HIV drugs had given American patients at least 3 million more years of life.
She worked with Dr. Ken Freedberg, a leading expert on how money is best spent in medicine.
“You can’t do everything,” Freedberg said, “and even if you could, you can’t do everything at once. So what Rochelle is particularly good at is understanding data about treatments and public health and costs, and putting those three sets of data together to understand, ‘Well, what do we do? And what do we do now?'”
So, if Walensky had a Wonder Woman superpower, it was using data to inform decisions and save lives. That analytic skill has come in handy over the past year, as she has helped lead the pandemic response for her Boston hospital and for the state of Massachusetts.
She has weighed in often — and publicly — about coronavirus policy and medicine, speaking to journalists with a seemingly natural candor that has contrasted with the stiffer style of some federal officials. In April, when a huge surge of covid cases hit, she acknowledged the pain.
“We are experiencing incredibly sad days,” she said in a spring interview. “But we sort of face every day with the hope and the vision that what we will be faced with, we can tackle.”
And in November, she offered a sobering reality check from the front lines about current covid medical treatments: “When I think about the armamentarium of true drugs that we have that benefit people with this disease, it’s pretty sparse,” she said.
Walensky published research on key pandemic topics, such as college testing and antibody treatments. And she weighed in often publicly — on Twitter, in newspapers and on radio and TV. Asked on CNN whether the President Joe Biden’s plan to get 100 million Americans vaccinated in 100 days could restore a sense of normalcy, she responded with characteristic bluntness — a quality that could cause trouble in these polarized times.
“I told you I’d tell you the truth,” she said. “I don’t think we’re going to feel it then. I think we’re still going to have, after we vaccinate 100 million Americans, we’re going to have 200 million more that we’re going to need to vaccinate.”
Walensky is facing a historic challenge and leading an agency for which she’s never worked.
Already, she’s fielded blowback for the new CDC guidance on when and how schools should reopen, and she’s openly worried about new, more transmissible variants spreading nationwide.
Still, Boston colleagues said they have no doubt that she’ll succeed in making the transition from leading an infectious diseases division of 300 staffers to a public health agency of about 13,000.
“I would lie down in traffic for her,” said Elizabeth Barks, the infectious diseases division’s administrative director at Mass General. “And I think our entire division would lie down in traffic for her.”
Leading and rebuilding the CDC in the midst of a pandemic will be difficult. But Barks and others who know Walensky well said she’s clear-eyed and ready to dig in to meet the challenge; she’ll try a new approach if first attempts fall short.
Walensky brought a plaque from her desk in Boston to CDC headquarters in Atlanta. It reads: “Hard things are hard.”
Cory Goldberg is a Kaiser Health News journalist.
This story is part of a partnership that includes WBUR, NPR and KHN.
'Forms a furry sphere'
Palomides
Purrless my cat can stroll away
Rejecting human cheer.
To the same corner wends its way
And forms a furry sphere.
How cordial is the mystery
Of feline solitude.
Until I beckon spaciously
And he returns for food.
— Felicia Nimue Ackerman.
This poem first appeared in the Emily Dickinson International Society Bulletin.